We’ve mentioned before that neurosurgery is one of the specialties that is embracing new and/or alternative technologies like augmented reality particularly strongly. One procedure performed by neurosurgeons pretty commonly is the placement of a parieto-occipital ventricular catheter. It is used to treat hydrocephalus, a condition that presents often in children (due to the occlusion of the Luschka and Magendie foramina), and sometimes in adults, after a severe head trauma. Either way, the condition is caused by accumulation of cerebrospinal fluid (CSF) into the ventricular system of the brain. CSF buildup in the skull leads to swelling and pressure, which is a medical emergency that can result in severe headaches, cognitive impairment, coma, and even death.
Hydrocephalus etymologically means “water on the brain.” The only way to treat it is to drain the excess fluid from the skull by placing a ventriculoperitoneal shunt (in the OR, under general anesthesia, for a permanent solution) or with a Parieto-occipital ventricular catheter, which is only a temporary solution. If the cause of the hydrocephalus has already been identified and resolved, there is no need to place a shunt. Because this treatment is so invasive but so critical for patients who need it, researchers from Jacksonville, Florida’s Mayo Clinic Department of Neurological Surgery have worked with researchers from the Emory University School of Medicine in Atlanta, Georgia to develop a solution.

The neuronavigation images that are routinely used during this type of operation were captured and transferred wirelessly to a head mounted display, the Google Glass. The surgeon wore a head mounted display that allowed them to search the radiologic studies in real time during the image-guided parieto-occipital ventriculoperitoneal shunt placement in two patients. Both procedures were completed successfully and with no complications, and correct catheter placement was confirmed.
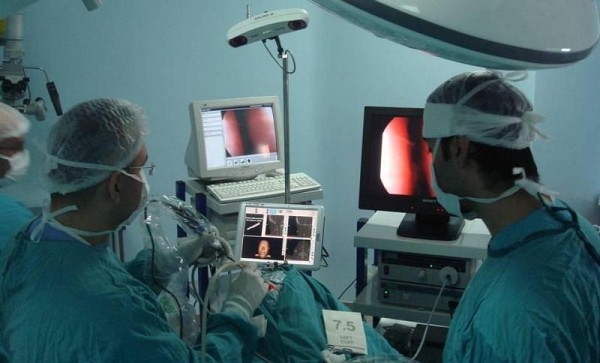
The head mounted display allowed the continuous monitoring of neuronavigation images in the upper right quadrant of the surgeon’s visual field. This reduces the need for the surgeon to turn their head to look at a monitor. While this might sound like a superficial problem, it’s really not just about comfort. Anything that causes the surgeon to break focus could be potentially harmful or even deadly to patients. This system is an example of a device that harnesses the power of visual imaging data to save patients’ lives.

As we have already stated, augmented reality and mixed reality have the potential to revolutionize surgical procedures, especially in the area of enhancing image-guided navigation. Of course, there’s more than one approach to this task–a superimposed image over the operating field can also provide incredible results for doctors. However, this could take years to perfect, and we want the technology to see some action now! We’d love to see more studies on this sort of thing, and especially focusing on reducing problems like fatigue. We think that the future of AR in neurosurgery is bright!
What do you think of it? Let us know in the comments section!








