We’ve already talked a bit about the benefits of plastic surgery for individuals who undergo it, whether for reconstructive purposes or strictly cosmetic ones. There is definitely a cultural influence–Western cultures have normalized it much more than other places in the world. We talked before about some uses for AR in plastic surgery, but we promised more, and we’re here to deliver! We think that there is a lot more to AR’s place in the profession of plastic surgery, and we’d like to talk about those perhaps less obvious applications.

First of all, we’d like to talk about a system built by the Institute of Biomedical Manufacturing and Life Quality Engineering and the School of Medicine, both at Shanghai Jiao Tong University in Shanghai, China. Researchers here have developed a workbench system equipped with a haptic feedback device, designed to teach and train surgeons to perform orthognathic maxillofacial surgery procedures with LeFort 1 procedures specifically in mind. These procedures are useful for mandibular malocclusion, facial asymmetry, obstructive sleep apnea, and maxillary atrophy. This system consists of a virtual imaging feature that utilizes mixed reality built from CT Scan DICOM imaging that resembles the operating field, and haptic tools built to provide the rest of the necessary surgical actions, such as bone sawing, drilling, and plate fixation. All of this is pulled together by haptic force feedback, which allows the trainee to have information about the procedure while they are performing it.
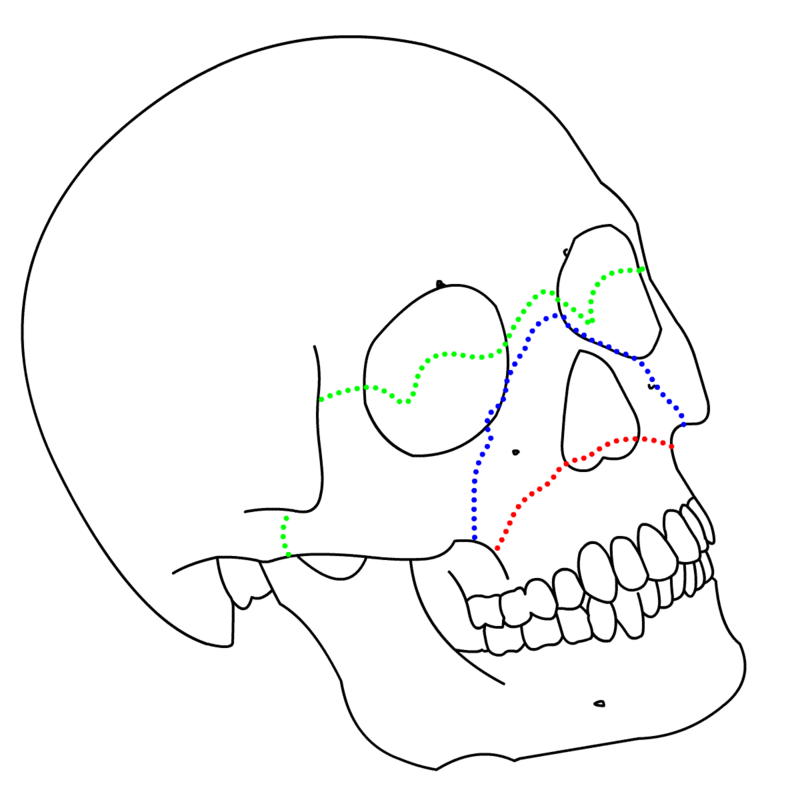
Image source: https://www.wikipedia.org/
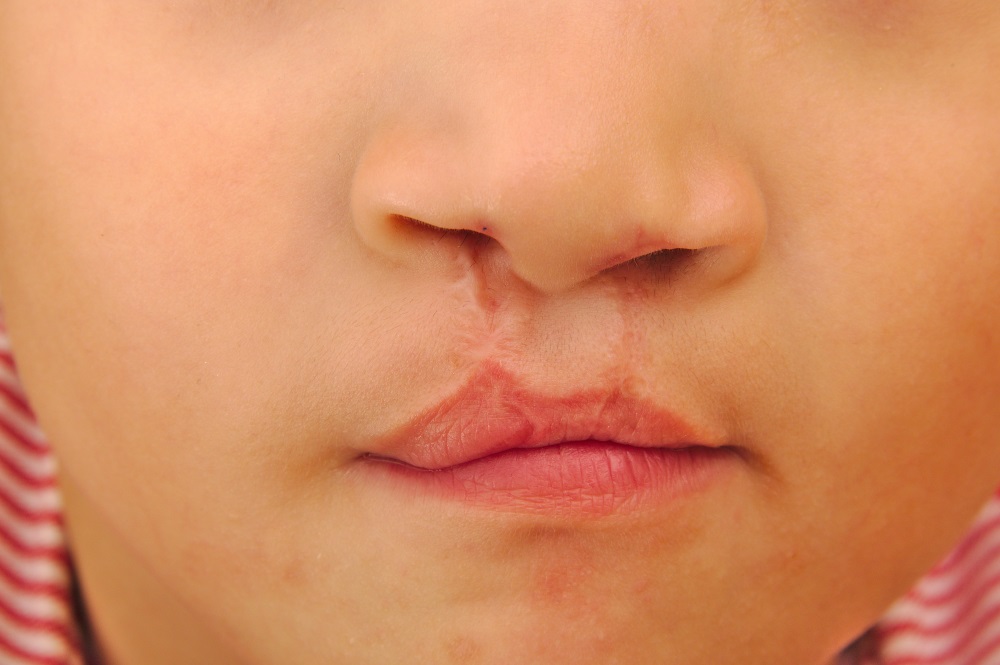
Moving right along, now we are going to talk about the National Biocomputation of Stanford University in California has recognized the worldwide issue that cleft palate presents. It’s one of the most common congenital abnormalities: the isolated form affects 1 in every 1509 babies born, and cleft lip with or without palate is even more common, affecting 1 in every 902 babies born in the US, according to The Cleft Lip and Palate Foundation of Smiles. This simulator uses haptic simulator and mixed reality technologies as the basic tools, engaging the user in an immersive and realistic training environment. Imaging was also generated through the 3D built models provided by CT Scan DICOM images, the difference being that the haptic feedback was built to emphasize the differences between tissues during the procedure. Overall, the technology was well-received, and proved itself to be a valuable training method.
We at ARinMED believe that AR and MR have so much to offer in the future for plastic surgery. Reminder that not all plastic surgery recipients are voluntary, cosmetic patients: many people who undergo plastic surgery do it for reconstructive reasons after accidents, trauma, or major illness. It can save lives and restore quality of life in people who have gone through terrible things. Many people after accidents are wary of plastic surgery: there is a sense of loss that a patient experiences knowing that they will look different, and many patients have anxiety about how they might look after the procedure. AR technology could help surgeons to provide a more realistic image of how the patient might look after surgery, and can help them to decide to have a surgery or to opt out. Plastic surgeons could also be able to offer their patients more clear ideas of how a procedure might look on their individual body or face, in real-time, and an image that is responsive to their movements, like an AR or MR reflection.
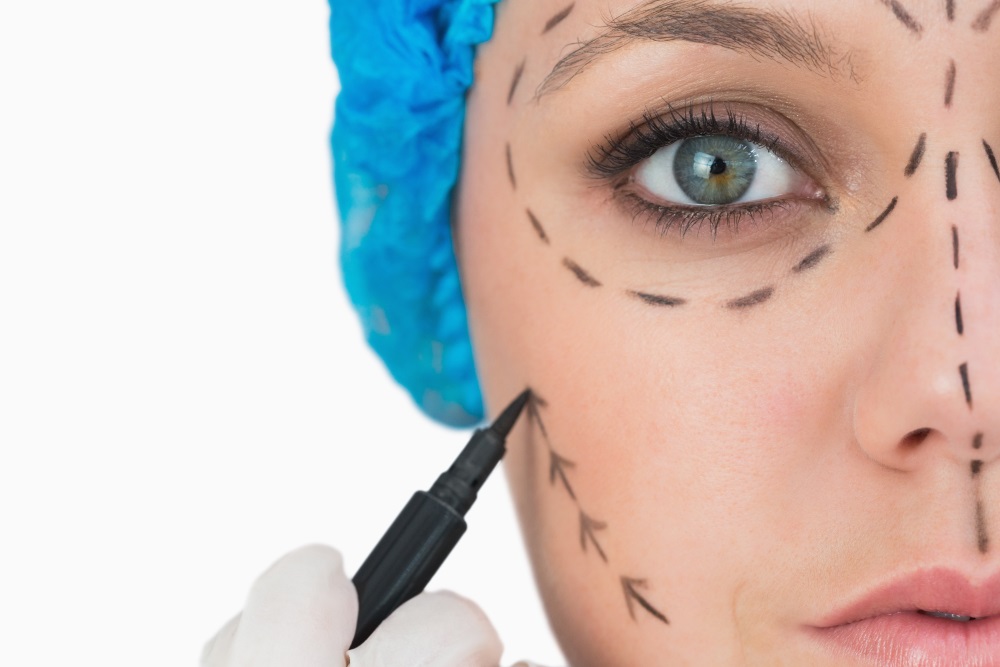
This isn’t the end of AR’s possibilities in plastic surgery. New technology could be developed to help the surgeon stay on track and ensure that the surgery looks just how the patient expects it to in the end, instead of the archaic method of writing on their skin. It could also allow for a more satisfying postoperative consult if the patient can see just how similar their face looks to the augmented image. What do you think about it? Are there other branches of medicine you’d like to see AR technology applied to? Please tell us your opinions, questions, and comments in the comments section below!








