Acetabular and pelvic fractures are some fairly serious orthopedic pathologies that are treated all over the world, even if they aren’t very common. Healthgrades reports that only one in 4,475 patients in the US suffers from a pelvic fracture, and only 10% of that number, according to the AO, will fracture the acetabulum, which is the socket in which the femur attaches. However, the prevalence isn’t the main issue here–it’s the impact this sort of injury has on a patient’s quality of life. Most of these patients are elderly, since aging can decrease the sturdiness of bones, and this type of injury doesn’t necessarily require a high impact or major trauma–a simple fall can cause it. Osteoporosis, which is more common in the elderly, increases the likelihood of this type of fracture, as well as the seriousness of the injury. Osteoporosis and other factors caused by aging can also make the reconstructive procedures more difficult and risky.

Keeping all of this in mind, researchers from the State Key Laboratory of Virtual Reality Technology and Systems of the Beihang University in Beijing, China have decided to address this issue. They have developed a system that allows the user to plan the reconstruction plate design for unilateral pelvic and acetabular fracture cases in the preoperative setting. All of this, of course, uses augmented reality techniques to improve the procedures required to repair these kinds of fractures, reducing invasiveness during the surgical procedure and respecting the patient’s morphology.
This proposal is composed of two subsystems. The first is a software that could be defined as a semi-automatic 3D virtual fracture reduction system. It serves to establish the type of pelvis that the patient has, and will help the physician to determine, through standardized criteria, the simplest way to treat the fracture. The second part of the software is a preoperative templating system that uses both virtual and real surgical implants. 3D models built from CT Scan data are taken, and the virtual fracture reduction system recognizes the anatomy of the patient and semi-automatically builds a “repaired” pelvis model. The software then facilitates the option for surgeons to plan the design and placement of the reconstruction plates in an interactive way. The average time required for this whole process from start to finish,including implant creation, is an impressive 10 minutes.
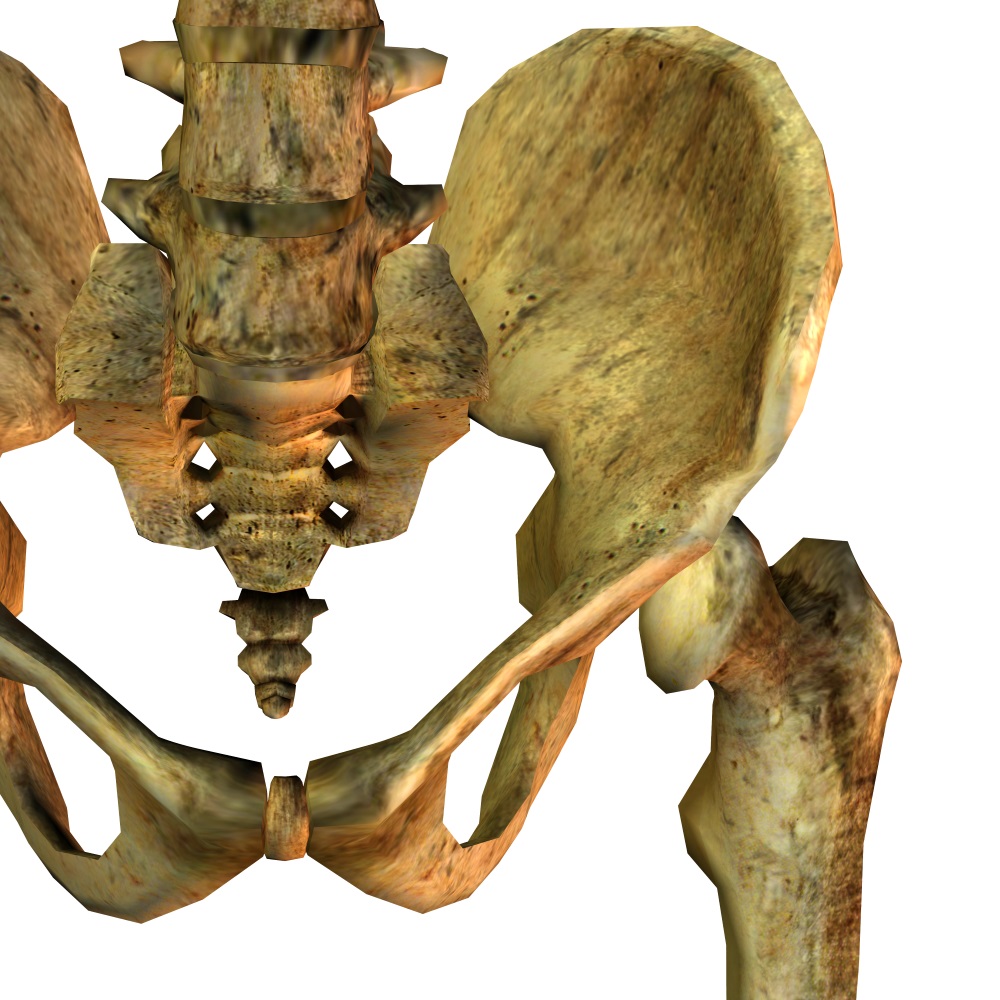
The second system in this proposal is where AR comes into the picture. The AR environment is set for surgeons to compare and match the actual implants to the digital ones.The system was applied in six clinical cases as a test, and we’re happy to say that it was a success for each one. Six minimally invasive surgeries were achieved using this system, with the variability of the virtual implant geometry being a mere 0.63 mm on average, with a standard deviation of 0.49 mm. We think that makes this study a success for Orthopedics and AR.

Of course, there’s always room for improvement. The integration of 3D printers into the system could allow the virtual prosthetic to be created directly from the one designed from the patient’s pelvis, which sounds pretty sci-fi, but it’s very feasible! We think this system could even undertake something bigger, like applications to other fractures in different parts of the body and different reconstructive surgeries. We’d love to see this system go worldwide and be a gold standard for treating fractures. With the right AR technology and the right people behind it, anything is possible.
Tell us what you think about it and voice your comments, questions, and concerns in the comments section!








