Imagine: It’s 3-am in the morning, a new critically ill patient arrives at the ICU and you have to work fast to save his life. Though your senses are not what they are at 8 am after a full night of sleep, you can rely on your training to be able to do an excellent job and perform all the procedures needed to save the patient’s life. Sometimes you need to use a nasogastric tube or a vesical probe, but most of the time, a central venous catheter (or central line catheter) must be inserted to administer vasoactive drugs and measure central venous pressure. It’s a very frequent and very dangerous procedure.

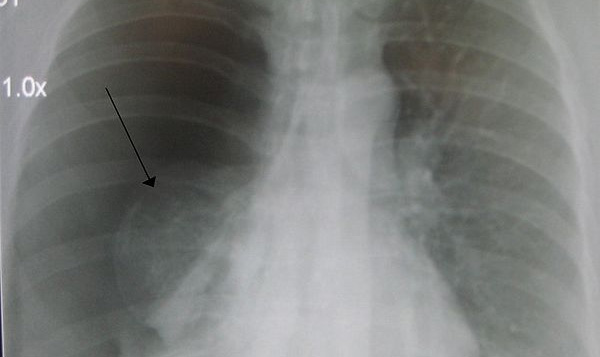
Pneumothorax, Hemothorax and vascular rupture, among others, are some of the most frequent complications that can arise when placing a central line catheter. Now we’re not saying these complications can be prevented, but with superior training, the risk of complications can be greatly diminished. As published by the Journal of the Society for Simulation in Healthcare (also published at NCBI), a team of physicians from the Department of Anesthesiology at the University of Michigan, and other collaborators are developing augmented reality based training designed to help physicians overcome some of the shortcomings of central line placement training that are inherent in mannequin-based training, including the inherent limitations of viewing internal anatomical structures during mannequin-based training.
For this study, the team used Augmented Reality glasses to display relevant internal anatomical landmarks on the mannequin and both experienced and inexperienced physicians tested the process. Interestingly, the results showed that the ability to successfully place the needle was amazingly similar between both experienced and inexperienced participants. The participants indicated that the AR technology was realistic (77.5%) and that the ability to view the internal anatomy through the AR tech was helpful (92.5%). This is a strong indicator that aspects of medical training may soon become far more efficient and intuitive through the use of AR technology.
As additional results come-in from research like this study, we expect Augmented Reality to become a much more integral part of medical training in the near future. Of course, as with all studies, further development and evaluation of this technology under a variety of simulated medical training settings is a must. Remember, the use of AR in medical training is in the first of what we hope will be several phases. But think of the possibilities this technology presents – in addition to the advancement in training that is sure to come through AR, what if we could use this technology to actually insert central line catheters on patients? subclavian? femoral? Anterior? posterior jugular? Although, we are likely some time away from these developments; these are legitimate possibilities. And these possibilities are the perspectives we like to imagine here at ARinMED. Send us a comment through our comments section and let us know what you think!
Sources: medlineplus.gov – 1, medlinplus.gov – 2, Journal of the Society for Simulation in Healthcare, National Center for Biotechnology Information







[…] which helps healthcare personnel locate veins for peripheral blood samples, and studies like this one which helps doctors learn to place a central line, are making vascular access more approachable and […]