Heart surgery has been one of the medical areas with some of the more impressive advances in the last century – from open heart surgery to transarterial procedures, from Edler and Hertz primitive cardiology to doppler echography, and so on. These efforts have focused on improving life expectancy, diagnosis time and quality of life for cardiologic patients. But it is safe to say that the continued improvement of every single aspect of cardiologic management is a must for modern cardiology, as every minute saved and every process improved can make a huge difference for each and every patient.
Transcatheter aortic valve implantation (TAVI), is a minimally invasive procedure that is a surgical alternative for patients with severe aortic stenosis. TAVI allows for a quick recovery rate and has far fewer potential complications than open heart surgery. However, TAVI relies on fluoroscopy and nephrotoxic contrast, which is a major cause for contraindicating this procedure for some patients. For example, many TAVI patients have underlying renal dysfunction and are therefore more vulnerable to acute kidney injury. The reported incidence of acute kidney injury after TAVI is between 12% and 57%.
During the last decade, relieving this procedure from the burden of fluoroscopy has been a recurring motive of study, and transesophageal echocardiography (TEE) has been the preferred method to apply as an alternative, but there has never been enough evidence to sufficiently prove that TEE is better than fluoroscopy.
Enter augmented reality (AR): where physicians at the Division of Cardiac Surgery of the Department of Surgery of the London Health Sciences Centre in Ontario, Canada; developed an alternative guidance system using AR and TEE based on the use of magnetic tracking sensors that were integrated into the TAVI catheter and TEE probe, which allowed these tools to be displayed in an AR environment. The precision of TAVI deployment using fluoroscopic guidance (the gold standard) was reported to be 3.4 mm, but the precision of TAVI using AR guidance was reported to be 2.9 mm, and its overall accuracy was 3.4 mm. This indicates that both perform similarly, or at minimum, that one of the methods is not substantially inferior to the other. Considering that one of the procedures doesn’t involve the use of nephrotoxic contrast nor the exposition to fluoroscopic radiation, it would be fair to think that the AR supported procedure had the upper hand in this study.
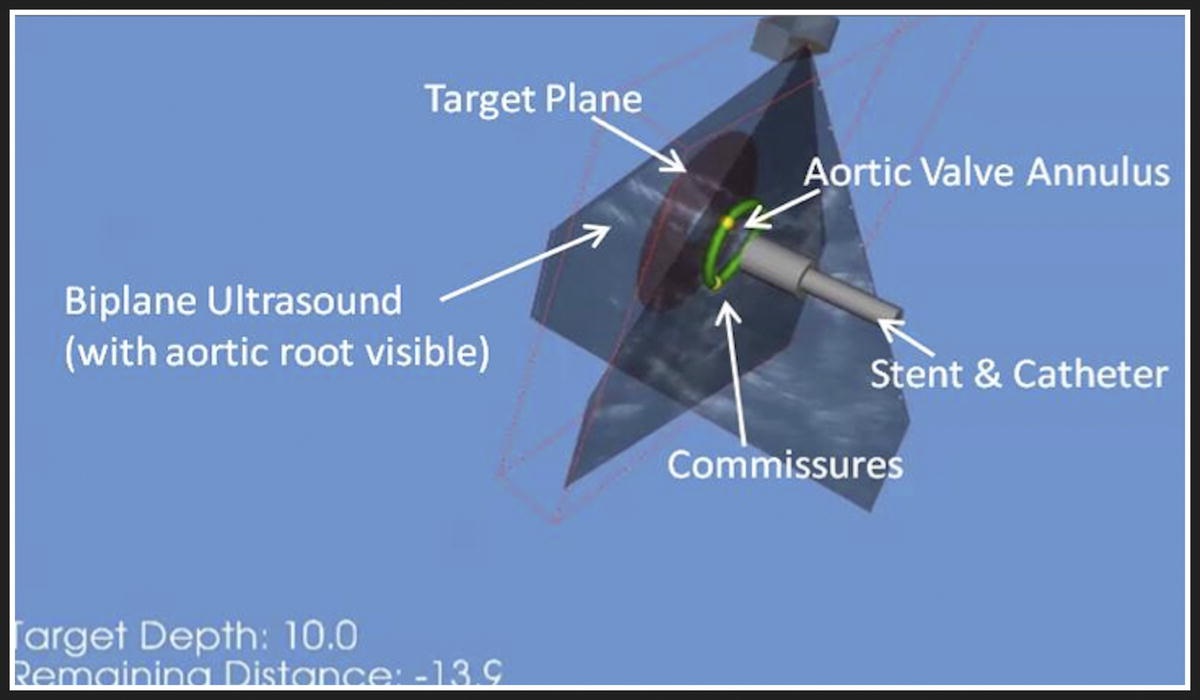
Optimal positioning and safe deployment of TAVI valved stents is integral to the success of the procedure, and more studies and procedural optimization (as explained in the study) and standardization needs to be done before it can become accessible outside an experimental context. But considering how the development of acute kidney injury is an important predictor of postoperative mortality, and that this study reveals that AR guidance system may achieve similar or better results than the gold standard while eliminating the use of nephrotoxic contrast and fluoroscopic radiation, here at ARinMED we are hoping that the studies to be done to make this procedure a reality continue at a rapid pace. Lives depends on it!!
Sources: LWW Journal, Europe PMC-1, Europe-PMC-2, WebMD, AHA Journals, FDA.gov, National Center for Biotechnology Information (NCBI)-1, NCBI-2, NCBI-3, NCBI-4, National Heart, Lung, and Blood Institute, London Health Sciences Center,








[…] and CT Scan have never been proven to be quite as accurate. Right now, AR is changing that with several studies that are currently in the works. It’s only a matter of time until AR imaging techniques are […]