Interventional medicine has become a trend into modern medicine; it’s easier, it’s faster, it’s a lot more practical, and results are seen immediately. Sounds pretty great right? Well, everything in this world has its pros and its cons and sadly, in most cases, a major challenge we face is radiation exposure. For instance, fluoroscopy is the technique used to make these procedures (such as Cardiac Catheterization), and it’s basically using x-rays to make real-time moving images, similar to getting many x-rays in a row.
The constant use of this technology puts physicians and other personnel, such as nurses and technicians, in real risk of developing certain types of cancer. Tissues like lymphoid tissue, thyroid, bone marrow, blood, testes, ovaries, and intestines are considered very radiosensitive, but not only to cancer. Cataracts and left-side brain tumors are some of the most worrying diseases emerging because of radiation exposure and there are protocols to be applied in order to decrease this risk, but can we do anything else? Physicians and engineers from Philips Research North America at Cambridge, Massachusetts think they can, let’s see what they bring to the table!

First of all, we must remember that X-ray exposure should be minimized by taking the measure of “as low as reasonably achievable” (ALARA) principle, which is basically the self-conscious measure that everybody should think in their own safety. But, this is more effective when radiation users in the room have a real and objective awareness of the radiation dose they are being exposed to, which is constantly changing. It depends on several factors, such as the position of the x-ray source, the position of its detector, what kind of procedure is being done, the position of other objects and people in the room, the use of protective clothing, etc. There are many things that people cannot be aware of at the moment of every single study.
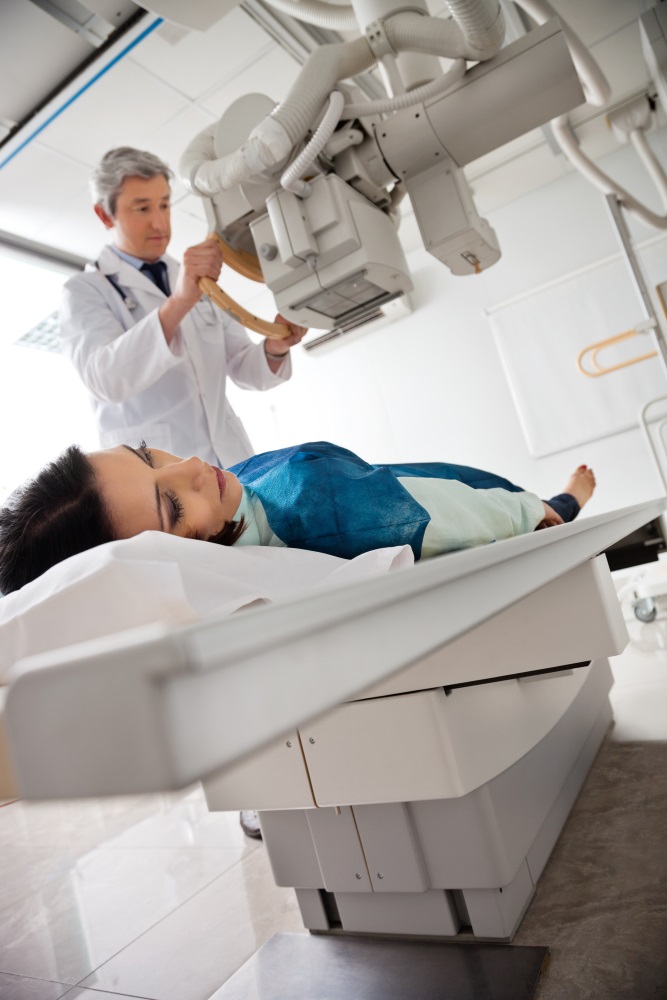
Then, Augmented Reality enters the frame and is applied by having personnel in the room who are exposed to radiation wear a real-time dosimeter badge that is wirelessly connected to a computer where data, such as cumulative and instantaneous dose information, is stored for each user in the room and then it is transmitted into a Microsoft HoloLens Head Mounted Display (HMD). The Microsoft HoloLens shows each user with a “virtual badge” that changes color and size in real time according to the radiation exposure, allowing the personnel in the room to make efficient and opportune changes to lessen the radiation exposure at the very moment of the procedure.
Seems like a very simple program, right? This program – if used correctly, will save lives, improve workflow and bring a new, powerful tool to the catheterization lab. Do you think there are other implications for this technology? Please leave your comments and feedback below!







