Lymphedema is a collection of lymph fluid, which results in swelling, most commonly in the limbs. One of the most common causes of lymphedema is the removal of a lymph node due to cancer treatment. While this treatment is unavoidable for many patients, the side effects can be devastating and really diminish the patient’s quality of life. Surgical treatment is available for this problem in the form of a lymphaticovenous anastomosis (LVA) surgery, which is a procedure which connects the remaining lymphatic vessels in an affected area of the body to the adjacent veins, allowing the lymphatic fluid to flow into the venous system and go back into circulation and to alleviate the swelling of the patient’s limbs.
lymphedema
During this surgery, infrared cameras are needed to perform indocyanine green lymphography (ICG), which helps the surgeon to identify the small vessels. This is difficult because they are thin, and the fluid inside them is transparent and faint in color, so surgeons cannot see it with just the naked eye. The problem is that during the surgery, surgeons must switch their focus back and forth from the operative field to the visual displays, usually placed on the wall or beside the operating table. This breaks the surgeon’s focus and can diminish the quality of the surgery, resulting in increased complications. To address this problem, physicians at the Hyogo College of Medicine in Nishinomiya, Hyogo, Japan decided to implement an augmented reality solution, in the form of a head-mounted device with a transparent display, allowing the surgeon to detect the infrared view and identify lymphatic vessels.
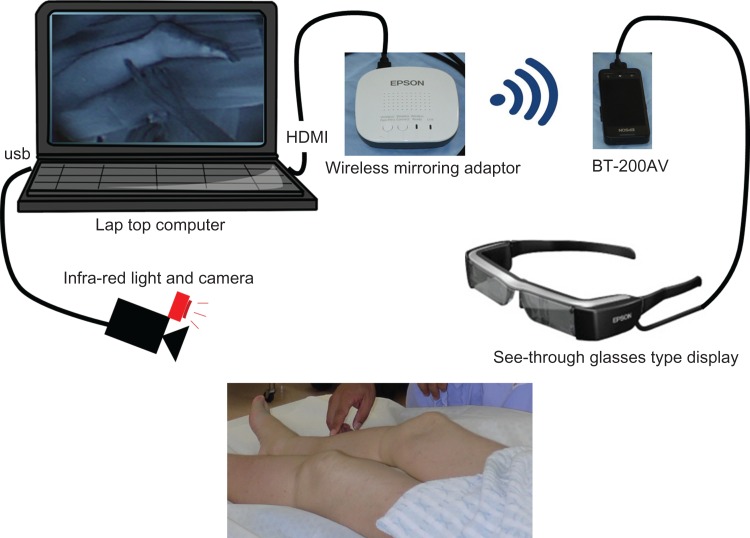
Thanks to AR, the infrared view is superimposed over the operative field, so that the surgeon can see both the real surgery and the infrared overlay at the same time, without taking their eyes off the procedure. Once the lymphatic vessels are detected by the infrared camera and marked by the AR system, the lymphaticovenous anastomosis can begin. Unfortunately, this system is not perfect–for example, there is still a lag between the real movement and the augmented image. As you can see in the displayed image, the infrared image is captured with the camera and then processed with a laptop computer to be transferred wirelessly to the head mounted display. The researchers unfortunately did not specify how severe this lag was.
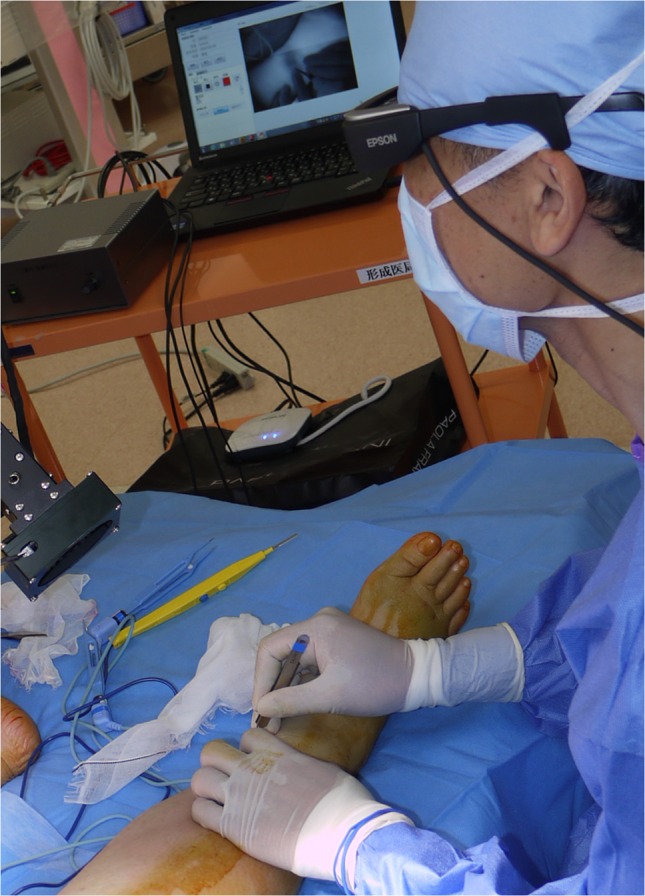
Speeding up the throughput speed might shorten the time lag, though there may be a limit to that, since the viewpoint of the camera is different from the one in the HMD, and because of this, the infrared view cannot be perfectly overlaid over the surgical area, which also means that the alignment will not be perfect. Another issue is that the surgeon reported that he was not comfortable using the 88g head mounted display (the Epson Moverio BT-200), which could also affect the surgeon’s concentration.

Despite these issues, we believe this is a great idea–it just needs some development. We certainly think that the researchers are on the right track and are doing a great job, but it’s always good to think about how things can be improved. We might suggest switching from a head mounted display to a device that could both detect and project at the same time, like a polished Kinect, for instance, in order to reduce issues with the point of view and the lag. Some of the newer HMD models have a shorter lag, but are still bulky and could be uncomfortable to wear for the duration of an entire surgery. We feel this analysis is missing a concrete statistical analysis of how the HMD and the system affected the surgery’s accuracy, but maybe that will come once some of the bugs are fixed. Hard numbers are essential in medicine! Anyway, it’s a great idea, and we look forward to watching this prototype reach its full potential

it can be done!
How excited are you for this system? Do you have ideas for how it could be improved? Let us know in the comments section!
Source: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4915215/







